Choose a country to view content specific to your location
H. pylori is 1 of 4 common infections that can lead to cancer- it is preventable with early detection.4
H. pylori is one of the most prevalent bacterial infections globally, characterized by typical gastrointestinal discomfort symptoms that can be treated. An H. pylori test is essential for accurate diagnosis and early intervention. When an H. pylori test is not conducted and the infection remains untreated, it may lead to the development of chronic gastritis, peptic ulcer disease, and even gastric cancer.5.
1 in 3 Americans are infected with H. pylori.1
9 in 10 ulcers are caused by untreated H. pylori infections.2
Gastric Cancer risk is 6 times higher in H. pylori-infected individuals.3
An H. pylori test is essential for detecting H. pylori, a bacteria linked to ulcers, gastritis, and stomach cancer. Early diagnosis with an H. pylori test helps prevent serious complications and ensures timely treatment. This H. pylori test is a simple, non-invasive procedure that provides accurate results for effective medical management. Regular H. pylori testing is recommended for individuals experiencing persistent digestive issues, as an H. pylori test can lead to early intervention and improved gut health.
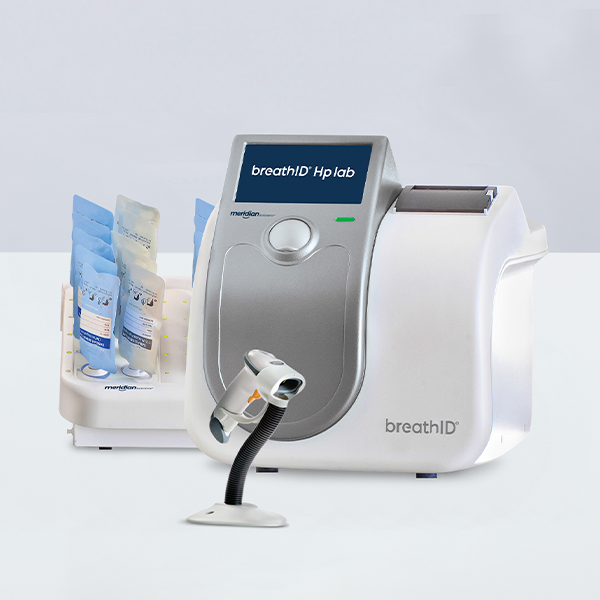
The BreathID® Hp Lab urea breath testing system detects H. pylori and confirms eradication for healthcare providers with large patient testing volumes.
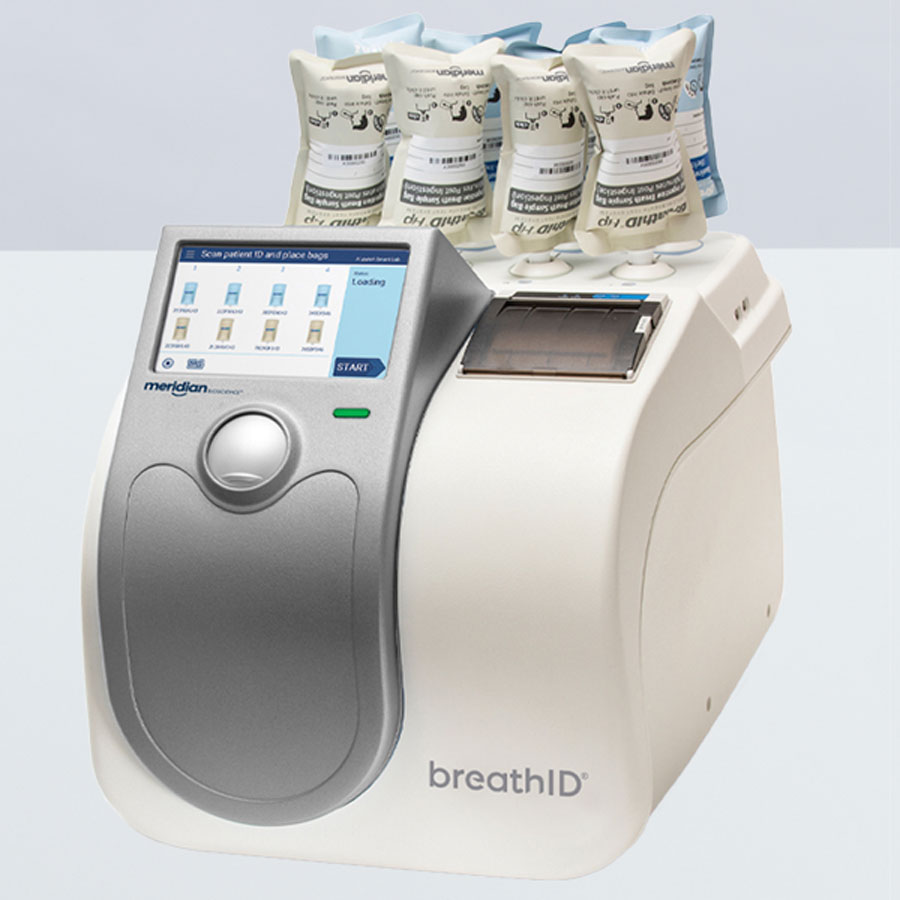
The BreathID® Smart urea breath testing platform detects H. pylori and confirms eradication for healthcare providers with mid-range patient testing volumes.

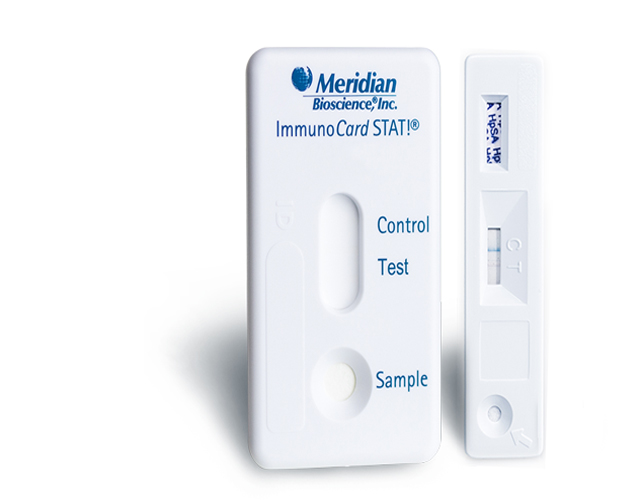

As dedicated partners in enhancing patient care, we take pride in our diverse diagnostic portfolio and go further by offering educational content and tools, leveraging our expertise to boost testing utilization and support our partners comprehensively.
H. pylori, or Helicobacter pylori, is a type of bacteria that infects the stomach lining and can lead to various digestive issues, including gastritis and peptic ulcers.
Dyspepsia, commonly known as indigestion, refers to discomfort or pain in the upper abdomen, often accompanied by symptoms like bloating, belching, and nausea. It can be caused by various factors, including overeating, eating too quickly, consuming fatty or spicy foods, stress, or underlying digestive disorders. Dyspepsia can sometimes be a symptom of an H. pylori infection or other gastrointestinal conditions. If symptoms persist or worsen, it’s important to consult a healthcare provider for proper evaluation and management.
H. pylori is usually transmitted through contaminated food, water, or utensils. It can also spread through close contact with an infected person’s saliva or vomit.
Individuals experiencing persistent abdominal pain, bloating, or other symptoms suggestive of a stomach ulcer or gastritis should consider getting tested for H. pylori. Those with a family history of stomach cancer or peptic ulcers may also benefit from H. pylori testing.
Approximately 50% of the world is infected with H. pylori. When left untreated, patients with H. pylori are at risk for long-term consequences such as ulcers and gastric cancer. Gastric cancer accounts for about 1.5% of all new cancers diagnosed in the United States each year. Early detection of H. pylori is vital in establishing appropriate treatment.1,6,7
Guidelines from AGA and ACG recommend a test, treat, and retest approach to confirm the eradication of H. pylori. Active infection tests such as 13C-urea breath tests or stool antigens are recommended rather than serology (antibody). Serology tests cannot determine active H. pylori infection and are no better than a coin toss in predicting the presence of active infection.5,7,8
A healthcare provider will determine the most appropriate treatment for H. pylori. However, treatment may typically involve a combination of antibiotics and acid-suppressing medications to eradicate the bacteria and heal any resulting ulcers. The specific regimen may vary depending on the individual’s health and other factors determined by their healthcare provider.
The ACG/AGA guidelines emphasize the need to test for diagnosis, treatment, and retest to confirm eradication using a non-invasive active infection test for H. pylori infection. H. pylori eradication therapy fails in 1 out of 4 patients. Antibiotic resistance and poor compliance are considered the most common causes of H. pylori treatment failure. There are ways to detect active infection and confirm infection eradication of an H. pyloriinfection with our non-invasive active infection tests that deliver trusted results – for lifelong impact.5
Yes, H. pylori infections can recur, especially if the initial treatment was not successful or if the individual is re-exposed to the bacteria. Follow-up testing may be recommended to ensure the infection has been completely eradicated as determined by a healthcare provider.
While it’s not always possible to prevent H. pylori infection, practicing good hygiene, avoiding contaminated food and water, and adopting safe food handling practices can reduce the risk of transmission. Additionally, avoiding close contact with individuals who have active H. pylori infections may help lower the risk.